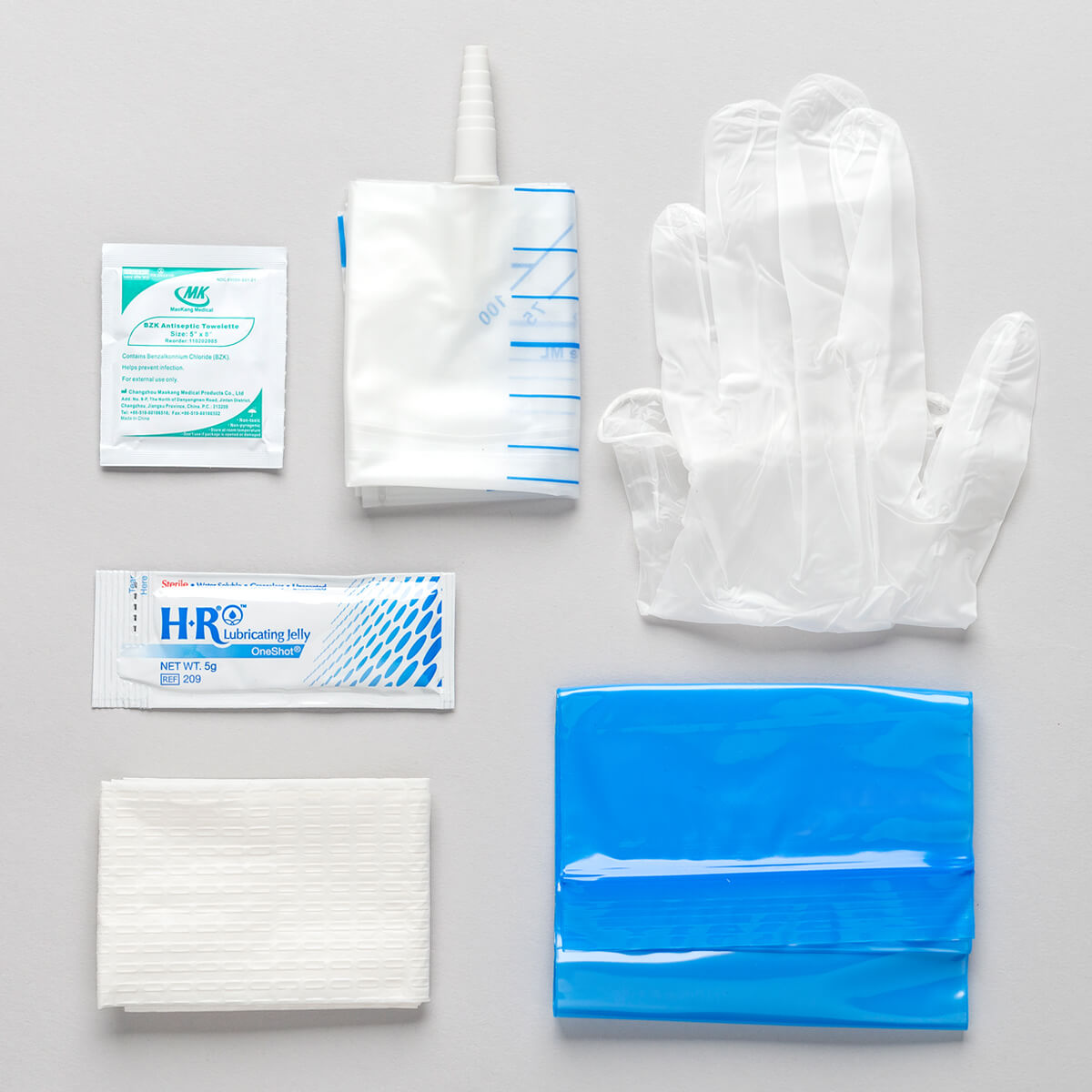
Urinary tract infection (UTI) is one of the most common healthcare associated infections with approximately half associated with the presence of a urinary catheter. surgery, inserting catheters and other devices), continence care, and avoiding breach in skin or mucous membranes. Relevant HCP behaviours include keeping hands, equipment and environments clean, observing IPC protocols during invasive medical procedures (e.g. primary, secondary and community care and nursing homes. Reducing the need for antibiotic use by preventing infections occurring requires behaviours to change in health care professionals (HCPs), patients and the general population across healthcare settings, e.g. 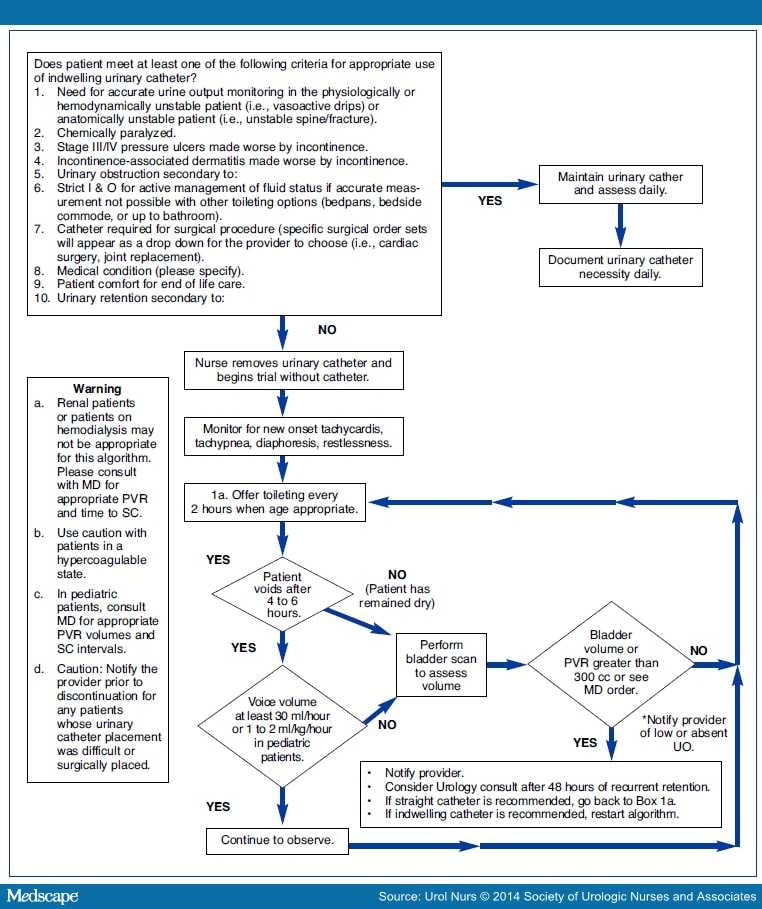
Improving infection prevention and control (IPC) is a crucial step in addressing the global health threat of antimicrobial resistance. This study suggests that targeting motivational, social and environmental influences may lead to more effective intervention design and refinement. 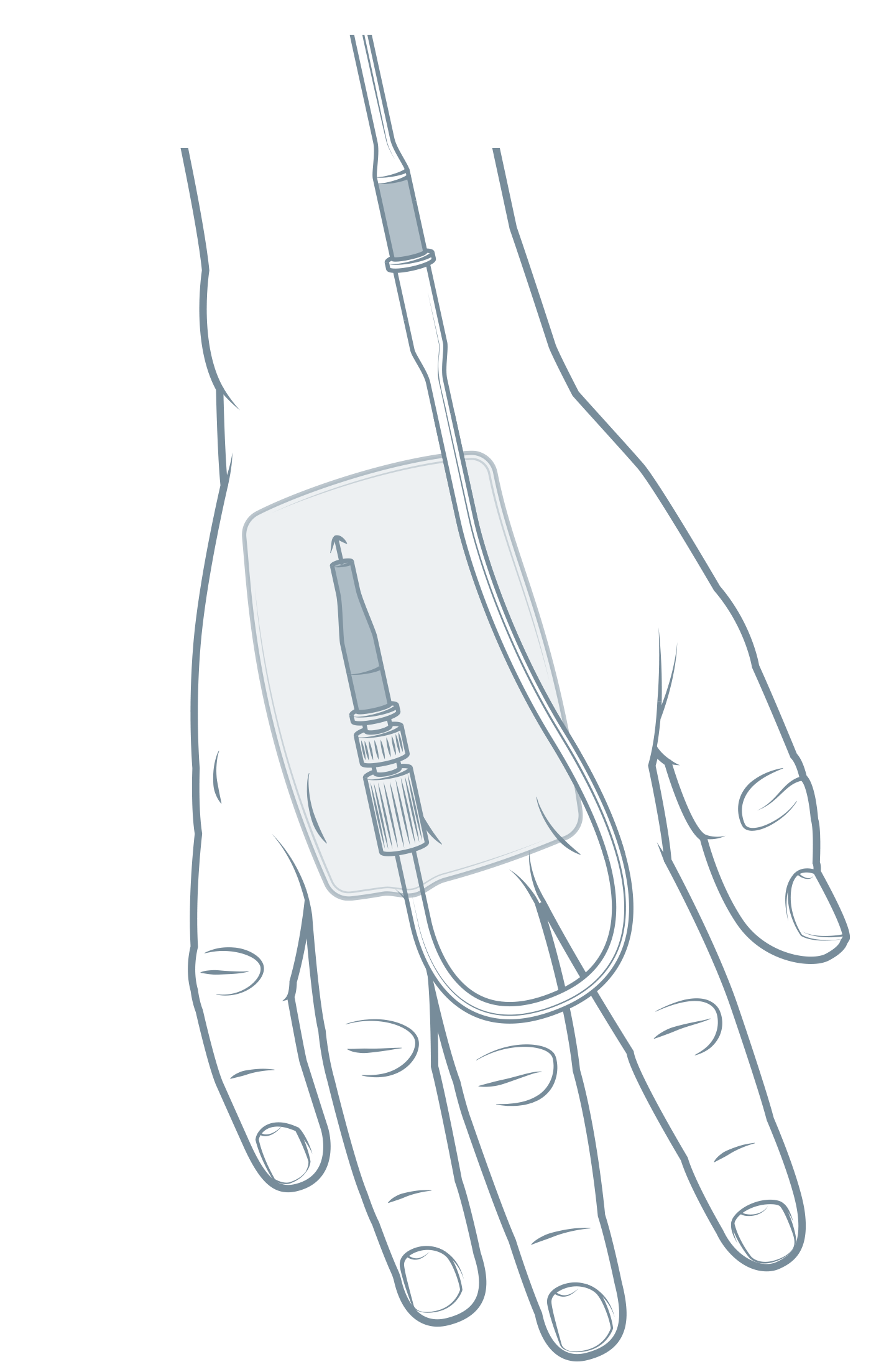
There were missed opportunities for intervention as most focus on shaping knowledge rather than addressing motivational, social and environmental influences. Interventions incorporated half the potentially relevant content to target identifed barriers to and facilitators of CAUTI-related behaviours. Social professional role and identity and environmental context and resources were targeted least frequently with potentially relevant BCTs. Interventions were primarily guidelines and included on average 2.3 intervention functions (1–5) and six BCTs (2–11), most frequently ‘education’, ‘training’ and ‘enablement.’ The most frequently used BCT was ‘information about health consequences’ which was used in almost all interventions. The most frequently reported barriers to and facilitators of CAUTI-related behaviours related to ‘environmental context and resources’ ‘knowledge’ ‘beliefs about consequences’ ‘social influences’ ‘memory, attention and decision processes’ and ‘social professional role and identity.’Įleven interventions aiming to reduce CAUTI were identifed. MethodsĪ mixed-methods, three-phased study: (1) systematic review of 25 studies to identify (i) behaviours relevant to CAUTI and (ii) barriers to and facilitators of CAUTI-related behaviours, classified using the COM-B model and Theoretical Domains Framework (TDF) (2) content analysis of nationally adopted CAUTI interventions in England identified through stakeholder consultation, classified using the Behaviour Change Wheel (BCW) and Behaviour Change Techniques Taxonomy (BCTTv1) and (3) findings from 1 and 2 were linked using matrices linking COM-B and TDF to BCW/BCTTv1 in order to signpost to intervention design and refinement. This strategic behavioural analysis applied behavioural science frameworks to (i) identify barriers to and facilitators of behaviours that lead to CAUTI (CAUTI-related behaviours) in primary, community and secondary care and nursing homes (ii) describe the content of nationally adopted interventions and (iii) assess the extent to which intervention content is theoretically congruent with barriers and facilitators. Interventions implemented nationally in England target behaviours related to catheter insertion, maintenance and removal, but the extent to which they target barriers to and facilitators of these behaviours is unclear. Catheter-associated urinary tract infection (CAUTI) is one of the most frequent device-related infections that may be amenable to prevention. Reducing the need for antibiotics is crucial in addressing the global threat of antimicrobial resistance.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
